 This year’s ACM MobiSys conference is in the Lake District in the UK. I really love this region in the UK. Already 15 years back when I studied in Manchester I often came up over the weekend to hike in the mountains here. The setting of the conference hotel is brilliant, overlooking Lake Windermere.
This year’s ACM MobiSys conference is in the Lake District in the UK. I really love this region in the UK. Already 15 years back when I studied in Manchester I often came up over the weekend to hike in the mountains here. The setting of the conference hotel is brilliant, overlooking Lake Windermere.
The opening keynote of MobiSys 2012 was presented by Dr. Paul Jones, the NHS Chief Technology Officer who talked about “Mobile Challenges in Health”. Health is very dear to people and the approach to health care around the world is very different.
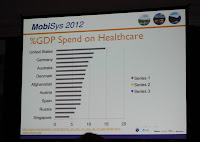 The NHS is a unique intuition that is providing healthcare to everyone in the UK. It is taxation funded and with its 110 billion pounds per year budget it is one of the cheaper (and yet efficient) health care systems in the world. The UK spends about 7% of its national cross product on health care, whereas the US or Germany nearly spend double of this percentage. Beside the economic size the NHS is also one of the biggest employers in the world, similar in size to the US department of defense and the Chinese people’s army. The major difference to other larger employers is, that a most part of the staff in the NHS is highly educated (e.g. doctors) and is not easily taking orders
The NHS is a unique intuition that is providing healthcare to everyone in the UK. It is taxation funded and with its 110 billion pounds per year budget it is one of the cheaper (and yet efficient) health care systems in the world. The UK spends about 7% of its national cross product on health care, whereas the US or Germany nearly spend double of this percentage. Beside the economic size the NHS is also one of the biggest employers in the world, similar in size to the US department of defense and the Chinese people’s army. The major difference to other larger employers is, that a most part of the staff in the NHS is highly educated (e.g. doctors) and is not easily taking orders
Paul started out with the statement: technology is critical to providing health care in the future. Doing healthcare as it is currently done will not work in the future. Carrying on will not work as the cost would not be payable by society. In general information technology in the health sector is helping to create more efficient systems. He had some examples that often very simple system help to make a difference. In one case he explained that changing a hospitals scheduling practice from paper based diaries to a computer based systems reduced waiting times massively (from several month to weeks, without additional personal). In another case laptops were provided to community nurses. This saved 6 hours per week and freed nearly an extra day of work per week as it reduced their need for travelling back to the office. Paul argued, that this is only a starting point and not the best we can do. Mobile computing has the potential to create better solutions than a laptop that are more fitting the real working environment of the users and patients. One further example he used is dealing with vital signs of a patient. Traditionally this is measured and when degrading a nurse is calling a junior doctor and they have to respond in a certain time. In reality nurses have to ask more often and doctors may be delayed. In this case they introduced a system and mobile device to page/call the doctors and document the call (instead of nurses calling the doctors). It improved the response times of doctors – and the main reason is that actions are tracked and performance is measured (and in the medical field nobody wants to be the worst).
Paul shared a set of challenges and problems with the audience – in the hope that researchers take inspiration and solve some of the problems 😉
One major challenge is the fragmented nature of the way health care is provided. Each hospital has established processes and doctors have a way they want do certain procedures. These processes are different from each other – not a lot in many cases but different enough that the same software is not going to work. It is not each to streamline this, as doctors usually know best and many of them make a case why their solution is the only one that does the job properly. Hence general solutions are unlikely to work and solutions need to be customizable to specific needs.
Another interesting point was about records and paper. Paul argued that the amount of paper records in hospital is massive and they are less reliable and save as many think. It is common that a significant portion of the paper documentation is lost or misplaced. Here a digital solution (even if non-perfect) is most certainly better. From our own experience I agree on the observation, but I would think it is really hard to convince people about it.
The common element through the talk was, that it is key to create systems that fit the requirements. To achieve this it seems that having multidisciplinary teams that understand the user and patient needs is inevitable. Paul’s examples were based on his experience of seeing the user users and patient in context. He made firsthand the observation, that real world environments often do not permit the use of certain technologies or create sup-optimal solution. It is crucial that the needs to are understood by the people who design and implement the systems. It may be useful to go beyond the multidisciplinary team and make each developer spending one day in the environment they design for.
Some further problems he discussed are:
- How to move the data around to the places where it is needed? Patients are transferred (e.g. ambulance to ER, ER to surgeons, etc.) and hence data needs to be handed over. This handover has to work across time (from one visit to the next) and across departments and institutions
- Personal mobile devices (“bring your own device”) are a major issue. It seems easy for an individual to use them (e.g. a personal tablet to make notes) but on a system-level they create huge problems, from back-up to security. In the medical field another issue arises: the validity of data is guaranteed and hence the data gathered is not useful in the overall process.
 A final and very interesting point was: if you are not seriously ill, being in a hospital is a bad idea. Paul argued, that the care you get at home or in the community is likely to be better and you are less likely to be exposed to additional risks. From this the main challenge for the MobiSys community arises: It will be crucial to provide mobile and distributed information systems that work in the context of home care and within the community.
A final and very interesting point was: if you are not seriously ill, being in a hospital is a bad idea. Paul argued, that the care you get at home or in the community is likely to be better and you are less likely to be exposed to additional risks. From this the main challenge for the MobiSys community arises: It will be crucial to provide mobile and distributed information systems that work in the context of home care and within the community.
PS: I like one of the side comments: Can we imagine doing a double blind study on a jumbo jet safety? This argument hinted, that some of the approaches to research in the medical field are not always most efficient to prove the validity of an approach.
